Radexpert
Approaches to interpretation of CT
Head
| Prior imaging | oldest & most recent PET, MRI |
| Scout | Lines, tubes, #'s, C-spine |
| Bone window | #'s, sinuses, lesions |
| Brain window | mass effect, blood (esp. SDH), edema, gray-white differentiation, CSF, arteries (aneurysms, calcifications) |
| Soft tissue window | Vessels, LN's, salivary glands, thyroid |
-
Chronicity of Hemorrhage
| 0 - 2 hrs | 40 - 60 HU |
| 3 - 48 hrs | 60 - 80 HU |
| 3 - 7 days | hyperdense core surrounded by hypodense halo |
| > 2 wks | hypodense |
Edema
Vasogenic:
Due to increased permeability of brain capillary endothelial cells to plasma proteins. Greatest in white matter. Astrocytes become swollen.
E.g. trauma, tumors, focal inflammation, and late stages of cerebral ischemia.
Cytotoxic:
Characterized by swelling of all the cellular elements of the brain. In the presence of acute cerebral ischemia, neurons, glia, and endothelial cells swell within minutes due to failure of ATP-dependent ion (sodium and calcium) transport. With the rapid accumulation of sodium within cells, water follows to maintain osmotic equilibrium. Increased intracellular calcium activates phospholipases and the release of arachidonic acid, leading to the release of oxygen-derived free radicals, and infarction.
E.g. various intoxications (dinitrophenol, triethyltin, hexachlorophene, isoniazid), Reye's syndrome, severe hypothermia, and early ischemia.
Spine
Critical spinal stenosis, AP dimension of thecal sac:
1.0 cm
1.4 cm in L-spine
Chest
| Prior imaging | oldest & most recent PET, MRI |
| Scout | Lines, tubes |
| Lung window | Airways: endobronch lesns bronchial wall thickening (wall thickness > diameter adjacent vessels) bronchiectasis (cylindrical, varicose, cystic)
Lung parenchyma: |
| Soft tissue window | Flow of contrast, heart, great vessels, LN's Abd (ascites, free air, vessels, adrenals, kidneys, spleen, pancreas) |
| Liver window | Liver (density, lesions, cirrhosis) |
| Bone window | Lines, #'s, lesions, invasn |
| Normal | Else
| Main PA < 3 cm
| Indicative of PA hypertension
| Aorta: | Root < 3.6 cm Ascending < 3.5 cm Proximal descending < 2.6 cm Distal descending < 2.4 cm Abd < 3 cm Aneurysm | If < 4 cm → ectasia If > 4 cm → dilatation
|
|
|
| |
Density > 200 HU indicates calcification
Cavity wall thickness:
< 2 mm, 95% benign
2 - 15 mm, 50% malignant
> 15 mm, > 95% malignant
Eccentric cavity or shaggy internal margins suggests malignancy.

Regional Nodal Stations for Lung Cancer Staging
(American Joint Committee on Cancer(AJCC) and the Union Internationale Contre le Cancer (UICC))
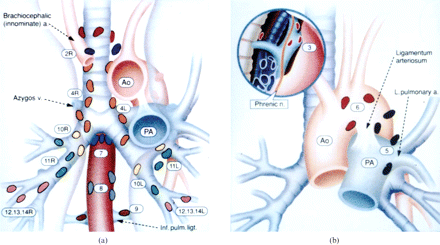
1 (red) = highest mediastinal nodes
2R and 2L (dark blue) = right and left upper paratracheal nodes
4R and 4L (orange) = right and left lower paratracheal nodes
7 (blue) = subcarinal nodes
8 (grey) = para-oesophageal nodes
9 (brown) = pulmonary ligament nodes
10R and 10L (yellow) = right and left hilar nodes
11R and 11L (green) = right and left interlobar nodes
12R and 12L (pink) = right and left lobar nodes
13R and 13L (pink) = right and left segmental nodes
14R and 14L (pink) = right and left subsegmental nodes
3 (pink) = pre-vascular and retrotracheal nodes
5 (black) = subaortic nodes
6 (red) = para-aortic nodes
Fleischner Society Recommendations for Incidental Pulmonary Nodule Follow-up
Multinodular Disease: A High-Resolution CT Scan Diagnostic Algorithm
Chest
PA
| Normal | Else
| Highest level of dome od diaphragm > 1.5 cm above line b/n costophrenic & vertebrophrenic junctions
| Empysema
| Paratracheal stripe < 10 mm
| CHF, lymphoma, bronchogenic cyst
| Main PA < 3 cm
| Indicative of PA hypertension
| |
Cavity wall:
< 5 mm → infection
> 10 mm → SCC
Vertebral body height decreased > 20% = compression #
If anterior → wedge #
If posterior → crush #
If middle → biconcave #
If adjacent endplate sclerosis → acute #
burst #
Chance #
Abdomen
| Prior imaging | oldest & most recent PET, MRI |
| Scout | Lines, tubes |
| Liver window | Density, lesions, cirrhosis |
| Soft tissue window | Skin, hernia,
adrenals, kidneys, spleen, pancreas,gallbladder, LN's ureters, bladder, bowel, terminal ileum, appendix prostate, seminal vesicles, uterus, ovaries |
| Bone window | #'s, lesions |
| Lung window | Lung bases |
-
Liver lesions
| Cyst | Thin, smooth wall 0 - 15 HU No enhancement No septations |
| Cavernous hemangioma | Discontinuous, nodular peripheral enhancement Centripetally-filling Isodense to aorta |
| Adenoma | Heterogen enhancement Well-defined capsule |
| FNH (fibrolamellar HCC similar) | Art phase: homogen enhancement (key) Solid (isodense when unenhanced) Central scar Radiating fibrous septa Portal venous phase: ↑ periph enhancement (dt lge pariph veins [no capsule]) |
Bosniak classification of cystic renal masses by CT scanning
| Category | Meaning | Criteria
| I
| Simple benign cyst
| Hairline thin wall
| Density less than 20 HU(similar to water) No septa, calcification, or solid components No enhancement II
| Benign cyst
| A few thin ( < 1 mm thick) septa
| No measurable enhancement (may be "perceived" enhancement) Includes uniformly high attenuation lesions <3 cm that are well marginated and do not enhance IIF
| Minimally complicated cyst that requires follow-up
| Multiple hairline thin septa or minimal smooth thickening of the wall or septa
| No measurable enhancement (may be "perceived" enhancement) Thick and nodular calcification of the wall or septa Totally intrarenal, nonenhancing, high attenuation lesions >3 cm III
| True indeterminate cystic mass that typically undergoes surgical evaluation
| Thickened wall or septa in which measurable enhancement is present
| IV
| Mostly malignant
| Enhancing soft-tissue components adjacent to, but independent of, wall or septum
| |
N.B. Enhancement = attenuation increase by at least 10 HU
Adrenal lesions
Nl limb 4 - 9 mm
| Adenoma | < 10 HU < 5 cm Sl enhancement Washout > 60% |
| Adenocarcinoma | usu > 5 cm Heterogen enhancement Calcifn in 30% - 50% |
| Metastasis | Usu bilat > 10 HU ↑ & heterogen enhancement Washout < 60% |
| Myelolipoma | < 0 HU |
Bowel Calliber
"3 - 6 - 9 - 12"
| Region | Max diameter
| Small bowel
| 3 cm
| Transverse colon
| 6 cm
| Cecum
| 9 cm
| Cecum b/f bursting
| 12 cm
| |
Small Bowel
"Rule of 3's"
-
Wall thickness < 3 mm
Fold thickness < 3 mm
Diameter < 3 cm
Air-fld levels < 3
Appendicitis
-
Appendocicolith
Diameter > 6 mm
Wall thickness > 2 mm
Enhancing wall
Peri-appendiceal fat stranding
Peri-appendiceal fld collection
Diverticulitis
-
Wall thickness > 3 mm
Peri-colonic fat stranding
Peri-colonic or intramural fld collection (abscess)
Approaches to interpretation of MRI
Head
| Time | Substance | T1W | T2W
| Hyperacute (< 12 hrs)
| oxy-Hb
| isointense
| hyperintense
| Acute (12 hrs - 3 days)
| deoxy-Hb
| isointense
| hypointense
| Early subacute (4 days - 1 wk)
| intracellular met-Hb
| hyperintense
| hypointense
| Late subacute (1 wk - 1 month)
| extracellular met-Hb
| hyperintense
| hyperintense
| Chronic (> 1 month)
| hemosiderin, ferritin
| hypointense
| hypointense
| |
DWI ↑
& ADC ↑
-
Vasogenic edema
T2 shine-through
-
Cytotoxic edema, e.g. acute ischemic stroke
Diffuse axonal injury
Abscess
Cerebritis
Epidermoid
| T1 ↑ | T1 ↓ | T1 ?
| T2 ↑
| gad | EC met-Hb hemangioma water | metastasis oxy-Hb
| T2 ↓
| flow (AVM, aneurysm) | dural calcifn IC met-Hb cortical bone | fibrous tissue hemosiderin, ferritin deooxy-Hb
| T2 ?
| fat (lipoma, dermoid) | proteinaceous fld (colloid cyst, craniopharyngioma, Rathke's cleft cyst) melanin (melanoma) post pit hvy metals |
Approaches to interpretation of Ultrasound
-
Echogenicity:
-
spleen = pancreas >
liver = left kidney >
right kidney
*** *** ***
thyroid >
muscle
Liver
-
Normal Liver
| Size | Length MCL < 15 cm |
| Parenchyma | Homogeneous |
| Surface | Smooth |
Lesions
| Cyst | Anechoic lumen, ↑ through transmission, well-defined back wall; Freq septn, puckering |
| Complex cyst | Internal echoes, thick wall, numerous or thick septns, solid elms, or calcifs E.g. hematoma, abscess, biloma, mets, echinococcus, tumor |
| Hemangioma | Hyperechoic, homogen |
| FNH | Isoechoic, spoke-wheel vascularity |
| Adenoma | Highly variable |
| HCC | V. variable. Includes target lesions |
| Mets | Usu target lesions, but v. variable |
| Lymphoma | Hypoechoic |
| Acute hepatitis | Starry sky (not specific) |
| Portal htn | Smg, ascites, portasystemic collaterals, reversal of portal venous flow |
Dilated Intrahepatic Ducts
-
> 2 mm diameter
> 40% diameter adjacent portal vein
↑ through transmission
Irreg, tort walls
Stellate config centrally
Enlarged GB
TIPS
-
Normal: 90 < shunt velocity < 190 cm/s
Shunt obstruction
Hep venous stenosis
Hep art pseudoaneurysm / art-portal fistula
Hematoma
Hemoperitoneum
Biloma
______________________________________________________________________________
Gallbladder
| Size | Transverse < 4 cm Longit < 10 cm |
| Wall thickness | < 3 mm |
| Lumen | Anechoic |
Gallbladder Intraluminal Abnormalities
| Stones | Shadowing, mobile |
| Polyps | Non-shadowing, non-mobile |
| Sludge | Non-shadowing, mobile |
Acute Cholecystitis
-
Wall thickness > 3 mm
Pericholecystic fld
Enlarged GB
Stones
Impacted stone
Sonographic Murphy's sign
GB Fossa Shadowing
| Shadow | Wall-echo-shadow complex | Back wall
| GB full of stones
| Usu clean
| Often
| Not seen
| Porcelain GB
| Variable
| Rare
| May be seen
| Intramural gas
| Usu dirty
| Rare
| May be seen
|
|
|
|
|
|
| |
Hyperplastic Cholecystoses
-
Cholesterolosis
Adenomyomatosis
-
Focal or diffuse mucosal hyperplasia & muscular layer thickening
Rokitansky-Aschoff sinuses - freq contain cholesterol crystals → comet-tail artefact
Common Duct
-
Diameter < 6 mm up to 60 y/o
then add 1 mm for every decade over 60 y/o
______________________________________________________________________________
Pancreas
-
Normal
-
Head < 3 cm
Body & tail < 2.5 cm
Duct < 3 mm; smooth
Homogeneous echotexture
Smooth or sl lobular surface
Acute Pancreatitis
-
↓ or heterogen echotexture
Enlarged
Fluid collections:
-
peripanc
perivascualar
periduodenal
retroperitoneal
Acute Pancreatitis Complications
-
Pseudocyst
Abscess
Necrosis
Biliary strictures
Venous thrombosis
Pseudoaneurysm
Chronic Pancreatitis
-
Calcifications
Dilated, irreg duct
Parenchymal atrophy
Solid, Hypoechoic Masses
-
Ca
Islet cell tumor
Lymphoma
Mets
Focal pancreatitis
Thrombosed aneurysm
Cystic Lesions
-
Pseudocyst
Macrocystic (mucinous) tumor [pre-malig or malig]
Microcystic (serous) tumor [benign]
Intraductal papillary mucinous tumor (IPMN)
Solid papillary epith neoplasm
Aneurysm or pseudoaneurysm
Cystic fibrosis
Autosomal domin polycystic dz
VHL
______________________________________________________________________________
Spleen
-
Normal
-
Longit < 13 cm
Width < 6 cm
Homogen echotexture
Smooth surface
Solid Lesions
-
Granuloma
Hemangioma
Hamartoma
Infarction
Abscess
Extramedullary hematopoiesis
Sarcoidosis
Lymphoma
Mets
Splenomegaly DDx
-
CHF
Portal htn
Leukemia
Lymphoma
Hemolytic anemia
Hepatitis
Mononucleosis
Generalized infection
- Uncommon:
Myelofibrosis
Glycogen storage dz
Malaria
Adrenal
-
Masses
-
Hemorrhage
Myelolipoma
Adenoma
Adenocarcinoma
Pheochromocytoma
Lymphoma
Mets
Kidney
-
Normal Length
-
Adult: 9 - 13 cm
Neonate: 43 mm (95% confidence limits 27 to 59 mm)
7 m/o: 61 mm (95% confidence limits 40 to 81 cm)
Urinary Obstruction
-
Hydronephrosis
Loss of ureteral jets
RI > 0.7
RI diff b/n Rt & Lt > 0.10
Hydronephrosis DDx
| Grade 1 | Grade 2 | Grade 3
| Mild
| Moderate
| Severe
| Sl distentn (pelvicaliectasis)
| Obvious diln; no cortical thinning
| Cortical thinning
| |
-
Obstruction
Previous obstruction
Extrarenal pelvis
Distended bladder
Pregnancy
- Uncommon:
Active diuresis
DI
Reflux nephropathy
Simple Cyst
-
Anechoic lumen
↑ through transmission
Well-defined back wall
No measurable wall thickness
Cystic disease
| Size | Tumors | Extrarenal cysts | Extrarenal lesions
| ADPKD
| Large
| 0
| Liver
| Cerebral aneurysms
| VHL
| Nl or lge
| RCC
| Pancreas
| Panc cystic neoplasms | Islet cell tumors Pheochromocytomas CNS hemangioblastomas Retinal angiomas Acq'd Cystic Dz of Dialysis | (ACD) Small
| RCC
| 0
| 0
| Tuberous sclerosis
| Nl or lge
| AML
| 0
| Cerebral hamartomas | Perivent nods LAM Cardiac rhabdomyomas
|
|
|
|
| |
Solid Masses
-
RCC
TCC
AML
Oncocytoma
Juxtaglomerular cell tumor (reninoma)
Lymphoma
Mets
Focal pyelonephritis
Focal parenchymal hypertrophy
Column of Bertin
Complex Cystic Masses
-
Hemorrhagic cyst
Hematoma
Multiseptated cyst
Infected cyst
Abscess
Multilocular cystic nephroma
Cystic RCC
Urothelial Thickening
-
Pyelonephritis
Ureteral stone/stent
Tpt rejection or ischemia
TCC
Pyelonephritis
-
Focal cortical ↑ or ↓ echogenicity
Renal enlargement
Urothelial thickening
Focal ↓ blood flow
Calculus
-
Echogenic reflectors
Acoutic shadow
Often twinkle artefact
Medullary Nephrocalcinosis
-
Medullary sponge kidney (tubular ectasia)
RTA
Hyperparathyroidism
Xanthogranulomatous Pyelonephritis (XGP)
-
Chronic obstruction → chronic UTI → lipid-laden macrophages → yellow inflammatory masses
US: Stone, caliectasis, perinephric inflam tissue & fluid
Transplantation
-
Urinary obstruction
Post-op fld collections (mass effect?)
-
Abscess
Hematoma
Lymphocele
Seroma
Urinoma
-
Stenosis
Thrombosis
A-V fistula
Pseudoaneurysm
Segmental infarction
-
Renal swelling
Enlarged hypoechoic pyramids
Focal cortical ↓ echogen
↓ visibility sinuses
RI < 0.7
Cyclosporin toxicity - similar to rejn
Infection - similar to rejn
PTLD
Bladder
-
Wall thickness
-
Well-distended < 3 mm
Poorly-distended < 5 mm
DDx:
Bladder outlet obstruction
Neurogenic bladder
Cystitis
Clots
Radiation
Neoplasia
-
TCC (90%)
SCC (5%)
Adeno Ca (2%)
-
Cortex echogen (>= spleen) or (> liver)
______________________________________________________________________________
General Abdomen
-
Bowel Wall Thickening
-
Edema
Inflammation
Infection
Ischemia
Hemorrhage
Neoplasm
Appendicitis
-
Diameter > 6 mm
Not compressible
Appendicolith
Hyperemia
Inflamed, echogenic periappendiceal fat
Adjacent fluid collections
Peritoneal Masses
-
Mets
Pseudomyxoma peritonei (from mucinous tumors)
Mesothelioma
TB
Omental infarction
Abdominal Wall Masses
-
Hematoma
Abscess
Seroma
Lymphocele
Demoid
Lipoma
Hernia
Endometriosis
Sarcoma
Mets
Lymphoma
______________________________________________________________________________
Scrotum
-
Testis
-
(4-5) x (2-3) x (2-3 cm)
(vol 15 - 20 mL)
homgeneous
smooth surface
Scrotal Lesion
| ↓ chance of neoplasm | ↑ chance of neoplasm
| Outside testis
| Inside testis
| Simple cyst
| Solid or cmplx cyst
| No detectable vascularity
| Detectable internal vascularity
| Non-palpable
| Palpable
|
|
| |
Enlarged, Hypoechoic Testis
| Blood flow | Tenderness
| Orchitis
| ↑
| yes
| Torsion
| ↓
| yes
| Lymphoma
| ↑
| no
| Seminoma
| ↑
| no
|
|
| |
______________________________________________________________________________
Thyroid
-
Normal
-
Isthmus < 4 mm
Lobes < 2 cm AP & transverse
Homogen
Hyperechoic to adjac muscles
Nodules
DDx: adenoma, colloid cyst, focal thyroiditis, Ca, lymphoma
| ↓ chance of Ca | ↑ chance of Ca
| Hyper- or isoechoic
| Hypoechoic
| Cystic elms
| Entirely solid
| Eggshell calcif
| Microcalcifs
| Inspissated colloid (colloid cyst)
| Cervical LAN
| No intranodal flow
| Intranodal flow
| Regular margins
| Irregular margins
| < 1 cm
| > 1 cm
| |
Metastatic LAN
-
Long-axis to short-axis <1.5
Oblitern echogenic hilum
Cystic changes
Microcalcifs
______________________________________________________________________________
Uterus
-
Normal (cm)
| Parity | Length | AP | Width
| 0
| 8
| 3
| 5
| 1
| 8.5
| 3.5
| 5
| 2-5
| 9.3
| 4
| 5.7
| > 5
| 9.7
| 4.2
| 6
|
|
|
|
| |
Post-partum Uterine Length (cm)
| 2 days | 3 weeks
| 18 - 23
| 10 - 12.5
|
|
|
|
|
|
|
|
| |
Endometrium (cm)
| AP | Descriptn
| Following menses
|
| Thin, hyperechoic line
| Prolif stage
| < 8 mm
| Thicker, uniformly hyperechoic line | Junctional zone visible Immed prior to ovuln
|
| Triple layer (3 hyper- sandwiching 2 hypo-)
| Secretory stage
| < 15 mm
| Thick, uniformly hyperechoic line
| Post-partum
| < 15 mm
|
| Post-menopausal
| < 5 mm (else, esp if vag bleed → endomet Bx)
| Thin, hyperechoic line
| |
______________________________________________________________________________
Adnexae
-
Ovary Upper limit of Normal (cm)
| L x W x AP | Volume (LxWxAP/2) | |
| Nullip, young adult | 3 x 3 x 2 | 9 |
| Parous | 5 x 3 x 2 | 15 |
| Perimenopausal | 9 | |
| 5 yrs post-menopausal | 5 | |
| 10 yrs post-menopausal | 3 | |
| > 15 yrs post-menopausal | 2 |
Most ovarian cysts in postmenopausal women are benign simple cysts.
If benign characteristics (unilocular, less than 5cm etc.), follow one additional time (e.g. 3 mos)
→ If no change, assume benign.
Follicles (cysts)
-
Dominant follicle < 2.5 cm
Functioning:
-
Affected by menstrual cycle
Usu < 25 mm
Simple:
- anechoic
↑ through transmission
No internal echoes
No wall thickening
-
Hemorrhagic cyst
Cystic teratoma (dermoid)
Endometrioma
Cystadenoma
Cystadenocarcinoma
Mets
| Wall thickness | |
| < 3 mm | 1 |
| > 3 mm | 2 |
| Mostly solid | 3 |
| Inner wall structure | |
| Smooth | 1 |
| Irregularities | 2 |
| Papillary projections | 3 |
| Mostly solid | 4 |
| Septa | |
| None | 1 |
| < 3 mm | 2 |
| > 3 mm | 3 |
| Echogenicity | |
| Anechoic | 1 |
| Low | 2 |
| Low with hyperechoic core | 3 |
| Mixed | 4 |
| Hyperechoic | 5 |
______________________________________________________________________________
First Trimester
MSD: mean sac diameter
| Gestational Age | Finding
| < 5 wks
| Intradecidual sac sign
| 5 wks (serum β-HCG 1000-2000 mIU/mL)
| MSD approx 5 mm (grows 1.1 mm/day)
| 5-6 wks
| Double decidual sac sign
| 5 - 8 wks
| HR > 100
| > 8 wks
| avg HR 140 (120-180)
| |
| Feature | Finding
| MSD 8 mm transvaginally or | 20 mm transabdominally (Serum β-HCG 7,200) Yolk sac visible
| MSD 16 mm transvaginally or | 25 mm transabdominally (Serum β-HCG 10,000) Embryo visible | (If not → 100% predictive of abnl IUP) Crown-rump length > 5 mm
| Cardiac activity
|
|
|
|
| |
Vaginal Bleeding
-
Implantation bleed
Subchorionic hemorrhage
Embryonic pregnancy/blighted ovum
Embryonic demise
Spontaneous abortion
Ectopic pregnancy
Molar pregnancy
Positive β-HCG and Empty Uterus
-
Early normal intrauterine pregnancy (<5 weeks)
Complete spontaneous abortion
Ectopic pregnancy
Sonographic Findings Associated with Ectopic Pregnancy
-
Embryo located outside of the uterus is 100% diagnostic of an ectopic pregnancy
Complex or solid adnexal mass
Moderate to large amount of pelvic free fluid, especially if particulate
Empty uterus in conjunction with serum β-HCG above level at which gestational sac should be seen.
Abortions
| Type of Abortion | Definition | Findings
| Blighted ovum
| Failed or abnormal embryonic development
| Empty gestational sac or sac with abnormal yolk sac and no embryo
| Embryonic demise
|
| No cardiac activity
| Threatened
| Vaginal bleeding + closed cervical os
| Ranges from live embryo to small, empty gestational sac to normal empty uterus
| Abortion in progress
| Intrauterine gestation in process of being expelled
| Irregular gestational sac in lower uterus/cervix +/- live embryo
| Incomplete
| Incomplete passage of gestational tissues
| Thickened endometrium +/- fluid and debris; areas of ↑ endometrial vascularity
| Complete
| Expulsion of all gestational tissues
| Normal empty uterus, may be mildly vascular
|
|
|
| |
Ultrasonography - Sample Reports
NORMAL RIGHT UPPER QUADRANT
-
TECHNIQUE: Real-time ultrasound evaluation of the right upper quadrant was
performed using a curved array transducer. Color Doppler imaging was used to
assess vascular flow.
DESCRIPTION: The visualized pancreas is normal.
The liver is homogenous in echotexture. No evidence of an intrahepatic mass or biliary ductal dilatation. Color Doppler interrogation of the main portal vein demonstrates hepatopetal flow.
The gallbladder is sonographically normal. The common duct is normal in caliber measuring ____mm in AP diameter.
Limited imaging of the right kidney demonstrates no hydronephrosis. No ascites in the visualized abdomen.
NORMAL LIVER DOPPLER
-
TECHNIQUE: Real-time ultrasound evaluation of the abdomen was performed utilizing a curved array transducer. Color Doppler imaging was used to assess vascular flow.
DESCRIPTION: The visualized liver and pancreas appear normal. Normal waveforms and appropriate direction of flow are identified in the following vessels: right, main and left hepatic arteries; right, main and left portal veins; right, middle and left hepatic veins.
Hepatopetal flow is demonstrated in the main portal vein, and the portosplenic confluence appears normal.
There is no ascites in the visualized abdomen.
IMPRESSION: Normal Doppler ultrasound of the abdomen.
RIGHT UPPER QUADRANT - PANCREAS NOT SEEN
-
DESCRIIPTION: The pancreas is not seen due to _____(overlying bowel gas OR body habitus).
IMPRESSION: Pancreas not seen. Otherwise, normal right upper quadrant ultrasound.
RIGHT UPPER QUADRANT - GALLSTONES
-
DESCRIPTION:
The gallbladder contains multiple shadowing stones in its dependent portion, but there is no evidence of gallbladder wall thickening or pericholecystic fluid. The common duct is normal in caliber measuring ____mm in AP diameter.
IMPRESSION: Cholelithiasis with no sonographic evidence of cholecystitis.
______________________________________________________________________________
NORMAL RENAL ULTRASOUND
-
TECHNIQUE: Real-time ultrasound evaluation of the kidneys and urinary
bladder was performed using a curved array transducer. Color Doppler imaging was used to assess vascular flow.
DESCRIPTION: Both kidneys are normal in size and echogenicity. The right kidney measures ___cm in long length, and the left kidney measures ___cm in long length. There is no evidence of hydronephrosis, mass, cyst or shadowing calculus.
Limited imaging of the urinary bladder demonstrates no abnormality. No ascites in the visualized abdomen and pelvis.
NORMAL RENAL ULTRASOUND WITH FOLEY CATHETER
-
DESCRIPTION:
The urinary bladder is decompressed by a Foley catheter and cannot be evaluated.
IMPRESSION:
1. Normal kidneys.
2. Foley catheter in place.
NORMAL RENAL TRANSPLANT ULTRASOUND
-
DESCRIPTION: The renal transplant is normal in size and echogenicity and measures ______cm in long length. There is no evidence of hydronephrosis, mass, shadowing calculus or peritransplant fluid collection.
Color Doppler imaging demonstrates normal arterial waveforms and arterial resistive indices, which range from 0._____ to 0._____.
Limited imaging of the urinary bladder demonstrates no abnormality. No ascites in the visualized abdomen and pelvis.
IMPRESSION: Normal ______renal transplant ultrasound.
ULTRASOUND OF TRANSPLANTED KIDNEY
TECHNIQUE: Real-time ultrasound evaluation of the transplanted kidney and urinary bladder was performed utilizing a curved array transducer. Color Doppler imaging was used to assess blood flow.
FINDINGS: The transplanted kidney is in the left iliac fossa and measures 10.7 cm longitudinally, which is within normal limits. Mild to moderate hydronephrosis is demonstrated. A small amount of anechoic fluid is adjacent to the inferior pole.
Arterial resistive indices are 0.67, 0.74, and 0.66. Venous flow is within normal limits. No evidence of stenosis, thrombosis or infarction. Renal cortex, pyramids and sinuses well visualized.
The urinary bladder is collapsed around a Foley catheter making assessment of the bladder suboptimal.
______________________________________________________________________________
NORMAL THYROID ULTRASOUND
-
TECHNIQUE: Real-time ultrasound evaluation of the neck was performed using a high resolution linear array transducer. Color Doppler imaging was used to assess vascular flow.
DESCRIPTION: Both lobes of the thyroid are homogenous in echotexture and normal in size. The right lobe measures ____x ____x ____cm. The left lobe measures ____x ____x ____cm. The isthmus measures ____mm in AP dimension.
There is no evidence of nodules. No extrathyroidal mass is seen.
Color Doppler imaging demonstrates normal vascularity of the gland.
IMPRESSION: Normal.
______________________________________________________________________________
NORMAL TRANSABDOMINAL & TRANSVAGINAL PELVIC ULTRASOUND
-
TECHNIQUE: Real-time ultrasound evaluation of the pelvis was performed using transabdominal and transvaginal approaches. Color Doppler imaging was used to assess vascular flow.
FINDINGS: The uterus is homogeneous in echotexture and normal in size measuring _____ x _____x _____cm. The endometrial stripe is normal in caliber measuring _____mm in the AP dimension.
Both ovaries are normal in size and appearance. The right ovary measures ____x _____x _____cm. The left ovary measures ____x ____x ____cm. Color Doppler imaging demonstrates arterial and venous waveforms in both ovaries. No adnexal masses are identified.
No free fluid in the cul-de-sac.
Limited imaging of the urinary bladder demonstrates no abnormality.
-
TECHNIQUE: Real-time ultrasound evaluation of the pelvis was
performed using transabdominal and transvaginal approaches. Color
Doppler imaging was used to assess vascular flow.
FINDINGS: Demonstration of a live, single intrauterine pregnancy with crown-rump length consistent with 8.5 to 9 weeks gestational age. Cardiac activity is demonstrated with a heart rate of 177. The gestational sac measures 3.1 x 2.9 x 4.1 cm. The uterus is homogeneous in echotexture and measures 10 cm longit x 6.1 cm in AP dimension x 6.8 cm transversely.
Both ovaries are small in size and with normal blood flow. The right ovary measures 2.1 x 2.5 x 0.9 cm. The left ovary measures 2.3 x 1.2 x 1.6 cm. No adnexal mass is present. No free fluid in the cul-de-sac.
IMPRESSION:
Live, single intrauterine pregnancy consistent with 8.5 to 9
weeks gestational age. Cardiac activity normal. No evidence of
ectopic pregnancy.
______________________________________________________________________________
NORMAL SCROTAL ULTRASOUND
-
TECHNIQUE: Real-time ultrasound evaluation of the scrotum was performed using a high resolution linear array transducer. Color Doppler was used to assess vascular flow.
FINDINGS: Both testes are homogeneous in echotexture and normal in size. The right testicle measures ___x ___x ___cm. The left testicle measures ____x ____x ___cm. No evidence of an intratesticular mass or abnormal calcification.
Color Doppler imaging demonstrates arterial and venous waveforms in both testes.
Both epididymides are normal in appearance, and there is no evidence of a hydrocele or varicocele.
IMPRESSION: Normal.
______________________________________________________________________________
NORMAL BABY HEAD ULTRASOUND
-
PORTABLE NEONATAL ECHOENCEPHALOGRAM
TECHNIQUE: Real-time ultrasound evaluation of the neonatal brain was performed using the anterior fontanelle as an acoustic window. Multiple sagittal and coronal images were obtained.
DESCRIPTION: The cortical sulcation pattern is within normal limits. OR The lack of cortical sulcation and wide cavum septum pellucidum is consistent with the patient's history of prematurity.
There is no evidence of acute intracranial hemorrhage, mass effect or midline shift. The ventricles are symmetric and normal in size and configuration.
IMPRESSION: No evidence of acute intracranial pathology.
______________________________________________________________________________
NORMAL COLOR DOPPLER IMAGING OF THE VEINS OF THE LOWER EXTREMITY
-
TECHNIQUE: Using duplex and color flow Doppler, the common femoral, superficial femoral and popliteal veins were evaluated in the (right or left) lower extremity. (or bilateral lower extremities)
DESCRIPTION: Normal flow, compressibility and augmentation are identified in the following visualized venous segments: common femoral vein; superficial femoral vein - proximal, middle and distal segments; and the popliteal vein.
There is no evidence of a Baker's cyst.
IMPRESSION: No evidence of a deep vein thrombosis in the visualized venous segments of the (right or left) lower extremity (bilateral lower extremities).
Procedure Notes
ULTRASOUND-GUIDED LIVER BIOPSY:
-
CLINICAL HISTORY:
PHYSICIANS:
TECHNIQUE:
18 gauge coaxial Temno biopsy instrument.
FINDINGS:
Three 18 gauge x 2 cm long core biopsy specimens taken to lab in formalin
COMPLICATIONS: None.
IMPRESSION: Ultrasound-guided liver biopsy without complications.
I personally supervised the performance of this procedure and reviewed and approved the report.
TECHNIQUE: With the patient sitting upright, real-time ultrasound examination of the left posterior chest was performed using a curved array transducer. At the point where the pleural effusion was deepest, the skin was marked with indelible ink.
FINDINGS: Moderate to large left pleural effusion. The skin was marked where effusion was deepest. Distance from skin to inner surface of chest wall was 2.5 cm. Distance from inner surface of chest wall to collapsed lung was approximately 7 cm.
IMPRESSION: Left pleural effusion assessed and skin marked for subsequent thoracentesis to be performed on floor by the clinical service. Patient tolerated procedure well.
Sample Normal Dictations
Format
-
EXAM:
COMPARISON EXAM:
CLINICAL HISTORY:
TECHNIQUE:
FINDINGS:
IMPRESSION:
Plain Radiographs
PA & LATERAL CHEST:
The cardiomediastinal silhouette is normal. The lungs are clear bilaterally. No pleural effusions, consolidations or evidence of congestive heart failure. The visualized osseous structures are unremarkable.
| Diffuse air-space opacities | "Diffuse, confluent opacities with ill-defined borders ..."
" ... in a perihilar (or lobar, segmental, etc.) distribution ..." " ... interspersed with small lucencies / air alveolograms / air bronchograms ..." " ... surrounded by acinar rossetes (opacities) ..." | Blood
Pus - e.g. bronchopneumonia, mycoplasma, viral, PCP Fluid - e.g. pulmonary edema (cardiogenic, non-cardiogenic) Cells - e.g. mets, lymphoma Protein - e.g. PAP |
| Multi-focal ill-defined opacities | "Multi-focal ill-defined opacities ..." (or "Patchy alveolar pattern ...") | Vasc: emboli (thromboembolic, septic), vasculitis (e.g. Wegener's)
Inf: e.g. bronchopneumonia, TB, fungal, PCP Iatro: drugs, radiation Neoplasia: e.g. mets, lymphoma, bronchioloalv cell Ca |
Airspace consolidations in adults must be followed to complete imaging resolution.
ACUTE ABDOMINAL SERIES:
The PA view of the chest demonstrates a normal cardiomediastinal silhouette. The lungs are clear bilaterally. No pleural effusions, consolidations or free air beneath the diaphragm.
The upright and supine view of the abdomen demonstrate a normal bowel gas pattern. There is no evidence of bowel obstruction or abnormal calcifications. The visualized bony skeleton is unremarkable.
FINDINGS: VP shunt begins in left lateral ventricle and exits cranium through right frontal craniotomy. It then travels down the subcutaneous tissues of the right side of the head, chest and abdomen and loops in the peritoneal cavity and finally terminates in the lower peritoneal cavity in the midline.
The VP shunt is intact. No discontinuity, obstruction, or kinking.
The visualized osseous structures and other structures including lungs and bowel gas pattern is within normal limits.
IMPRESSION: VP shunt intact and patent.
GENERAL MSK:
No fractures, subluxations, abnormal calcifications, radio-opaque foreign bodies, effusions, or soft tissue swelling.
FIVE VIEWS OF THE CERVICAL SPINE:
-
Can only evaluate from C1 to C6. No acute fracture or subluxation. If cannot clear clinically, should repeat study or do CT.
The spinal alignment, vertebral body heights and disk spaces are within normal limits. There is no evidence of acute fracture or dislocation. There is no prevertebral soft tissue swelling. The distance between the odontoid process and anterior arch is within normal limits. The neural foramina are patent bilaterally.
THREE VIEWS OF THE LUMBOSACRAL SPINE:
There are five lumbar type vertebral bodies. The spinal alignment, vertebral body heights and disk spaces are within normal limits. No acute fracture or spondylolisthesis. The sacroiliac joints are intact bilaterally.
Discogenic vertebral sclerosis involving the superior aspect of L4 and inferior aspect of L3.
FOUR VIEWS OF THE KNEE:
"Findings compatible with prior ACL repair."
"Limited views of left knee do not reveal any gross abnormalities."
FOUR VIEWS OF THE ANKLE:
There is no evidence of acute fracture or dislocation. No significant soft tissue swelling, joint effusion, abnormal calcifications or radio-opaque foreign bodies. The base of the fifth and ankle mortise is intact.
Possible pes panus deformity, though the lateral view is non-weight bearing, thus this cannot be confirmed with certainty.
Recommend MRI if concern about osteomyelitis.
There is an ill-defined, moth-eaten lesion in the upper right humerus with a pathological fracture running transversely through it. There is periosteal reaction with Codman�s triangles on the superior part of the lesion.
Imp: Aggressive neoplasm in proximal humerus. Pathological fracture in same location. Most likely etiology is metastatic disease. Also should consider a primary neoplasm. Consider MRI for further characterization, and bone scan to assess for additional lesions.
Degenerative joint disease is present in the right acromioclavicular joint. There are also findings suggestive of rotator cuff disease on the greater tuberosity of the humerus.
The third digit of the right hand demonstrates diffuse soft-tissue swelling, predominately along the proximal interphalangeal joint. There is diffuse DIP and PIP joint degenerative joint disease. The DIP joint in the third digit demonstrates changes that are likely related to osteophytes. No erosion is present. No evidence of osteomyelitis. There is severe DJD in the first carpometacarpal joint.
IMP: Changes in DIP in third digit likely related to osteophytes. There is diffuse degenerative joint disease in the DIP and PIP joints. No evidence of septic arthritis, osteomyelitis, or gout. If concerned about gout, can correlate with serum uric acid level.
CT
CT HEAD:
-
TECHNIQUE: Contiguous axial images using 4.8 mm collimation from vertex of the skull to the base of the skull. No contrast was used.
FINDINGS: The ventricular and cisternal spaces are normal in size, shape and configuration for a patient of this age. No dominant mass, midline shift or hydrocephalus. No intracranial hemorrhage or extra axial fluid collections. No abnormal areas of increased or decreased attenuation within the brain parenchyma. (If the examination was performed with contrast: There are no abnormal areas of contrast enhancement.)
The visualized skull is intact. The intraorbital contents are within normal limits. The visualized paranasal sinuses and mastoid air cells are clear.
IMPRESSION: Normal (enhanced) or (unenhanced) CT scan of the head.
The basilar cisterns are intact.
Evidence of an old infarction in the left MCA territory with ex vacuo dilatation of the adjacent lateral ventricle.
There is an area of decreased attenuation within the left frontal region superior to the sylvian fissure. This may represent an area of new edema or ischemia.
centrum semiovale
concha bullosa
Haller cell
resection of uncinate process and maxillary antrectomy
********************
There is acute blood in the suprasellar cistern and adjacent cisterns and in the sylvian fissures consistent with a subarachnoid hemorrhage. The temporal horns of the lateral ventricles are mildly dilated suggesting early hydrocephalus. The ambient cisterns and adjacent cisterns are not well visualized, which is suggestive of brain parenchymal swelling.
No dominant mass or midline shift. Differentiation between gray matter and white matter is still maintained.
vasogenic edema or glial infiltration or gliosis in right parietal region.
There is a hyperattenuating 8.7 mm lesion in the right posterior parietal area (image #24). This could represent a small hemorrhage versus tumor nodule.
TECHNIQUE: Contiguous axial images using 2 mm collimation from aortic arch to orbits following intravenous administration of contrast. Coronal and sagittal reconstructions done.
FINDINGS: Stable low-density lesion in right lobe of thyroid gland measuring 0.8 cm, likely representing nodule, cyst or adenoma.
Visualized upper lungs are clear. Visualized heart and mediastinum are unremarkable.
Intra-orbital contents within normal limits. Visualized osseous structures and visualized intracranial structures unremarkable. Paranasal sinuses, mastoid air cells and middle ears clear. No asymmetry in pharynx.
CHEST CT WITH (OR WITHOUT) CONTRAST:
-
TECHNIQUE: Helical images with 10 mm colimation were obtained from the thoracic inlet through the adrenal glands (following the administration of intravenous contrast) or without the use of intravenous contrast.
FINDINGS: There is no axillary, mediastinal, or hilar lymphadenopathy. The heart and great vessels are within normal limits.
The lungs are clear bilaterally. No pulmonary nodules, infiltrates, or pleural effusions.
The visualized upper abdominal structures are within normal limits.
No sclerotic or lytic lesions are identified within the visualized osseous structures.
CT OF THE ABDOMEN WTH CONTRAST:
-
TECHNIQUE: 10-mm contiguous axial sections were obtained from the dome of the diaphragm through the iliac crest. IV and enteric contrast were administered. Non-ionic contrast was used due to known safety conferred by the use of non-ionic contrast relative to ionic contrast material.
FINDINGS: The visualized lung bases are clear. The visualized heart and posterior mediastinal structures are within normal limits.
Intra-abdominally, the liver, gallbladder, pancreas, spleen and adrenal glands are within normal limits. There is no retroperitoneal or mesenteric lymphadenopathy. The visualized loops of small bowel and large bowel are within normal limits. No free fluid or free air within the visualized abdomen.
CT OF THE ABDOMEN & PELVIS WITH CONTRAST:
-
TECHNIQUE: Contiguous axial images using 5 mm collimation from the dome of the diaphragm to the ischial tuberosities following administration of intravenous and enteric contrast.
FINDINGS: The visualized lung bases are clear. The visualized heart and posterior mediastinal structures are within normal limits.
Intra-abdominally, the liver, gallbladder, pancreas, spleen, kidneys, and adrenal glands are within normal limits. No retroperitoneal or mesenteric lymphadenopathy. The visualized loops of small and large bowel are unremarkable. No free air or free fluid within the abdomen or pelvis.
Within the pelvis, the bladder, uterus (or prostate and seminal vesicles) and rectum appear within normal limits. No pelvic lymphadenopathy.
Visualized osseous structures unremarkable. No sclerotic or lytic lesions identified.
CT for Appendicitis
TECHNIQUE: Contiguous axial images from dome of diaphragm to ischial tuberosities using 5 mm collimation after intravenous and oal administration of contrast. 2 mm axial reconstructions performed through the right lower quadrant. 2 mm coronal reconstructions performed through the abdomen and pelvis. Delayed images of the pelvis also obtained with 2D reformats.
FINDINGS: Retrocecal appendix noted in the right lower quadrant; 9 mm in diameter, fluid-filled, and the wall enhances with contrast. No appendicolith is seen. No periappendiceal abscess or fluid collections. No gas within lumen of appendix. Delayed images show well opacified cecum and ascending colon but no contrast or air in the appendix.
IMPRESSION: Findings are suspicious for early appendicitis.
Equivocal for acute appendicitis. Recommend delayed images when contrast has entered the cecum.
Flouroscopy
BIPHASIC ESOPHAGRAM:
-
TECHNIQUE: EZ gas crystals followed by barium were administered orally and multiple spot films of the esophagus were obtained in various projections.
FINDINGS: The caliber, mucosal pattern, and peristalsis of the esophagus are normal. No ulcerations, filling defects, or strictures. No hiatal hernia or gastroesophageal reflux.
MODIFIED BARIUM SWALLOW WITH SPEECH THERAPY:
-
TECHNIQUE: Lateral video fluoroscopy was performed in conjunction with Speech Therapy. Multiple consistencies were used to evaluate swallowing function.
FINDINGS:
Oral phase: Mastication. Bolus formation.
Premature spill over. Aspiration before swallow.
Pharyngeal phase: Laryngeal elevation. Epiglottic excursion.
Vallecullar / pyriform residue.
Penetration. Aspiration. Cough response.
Esophageal phase: Stricture. Diverticulum. TE fistula.
IMPRESSION: Moderate oral and pharyngeal dysfunction. See Speech Pathology report for recommendations.
BIPHASIC UPPER GI:
-
TECHNIQUE: EZ gas crystals followed by barium were administered orally and multiple spot films of the esophagus, stomach and proximal duodenum were obtained in various projections.
FINDINGS: The peristalsis, mucosal pattern and caliber of the esophagus are normal. No hiatal hernia or gastroesophageal reflux.
The caliber and mucosal pattern of the stomach is normal. No ulcers or filling defects.
The proximal duodenum is normal. No ulcers or filling defects.
SMALL BOWEL FOLLOW THROUGH:
-
TECHNIQUE: A scout film of the abdomen was obtained. Barium was then administered orally and multiple sequential overhead films of the abdomen were obtained over a time period. Spot films of the terminal ileum were then obtained.
FINDINGS: The scout film of the abdomen demonstrates a normal bowel gas pattern. No abnormal calcifications or evidence of bowel obstruction.
The transit time of the barium from the stomach to the cecum was approximately . The peristalsis, mucosal pattern, caliber, and orientation of the duodenum, jejunum and ileum are normal. No strictures, filling defects, ulcers or fistulas. Spot films of the terminal ileum demonstrate no abnormality.
TECHNIQUE: A scout film of the abdomen was obtained. The barium enema tip was inserted into the rectum by the technologist and the balloon inflated by the radiologist under fluoroscopy. Barium was then administered and flowed freely to the cecum. While the barium flowed in, spot films of the colon were obtained intermittently. This was then followed by overhead films of the abdomen in various projections.
FINDINGS: The scout film of the abdomen demonstrates a normal bowel gas pattern. No evidence of bowel obstruction. No abnormal calcifications.
The barium flowed freely to the cecum without reflux into the terminal ileum. There are innumerable diverticula in the sigmoid and descending colon. No evidence of diverticulitis. No evidence of perforation or abscess. Otherwise, the caliber and haustral pattern of the colon is within normal limits. No obvious polyps or masses are seen. No strictures, filling defects, or ulcerations. Spot films of the cecum demonstrate a competent ileocecal valve.
IMPRESSION:
1. Severe diverticulosis without evidence of diverticulitis or other abnormalities. Note that single contrast barium enema is insensitive at detecting mucosal abnormalities. If this is a concern, a double contrast barium enema is recommended.
DOUBLE CONTRAST BARIUM ENEMA:
-
TECHNIQUE: A scout film of the abdomen was obtained. The barium enema tip was then inserted into the rectum by the technologist and the balloon inflated by the radiologist under fluoroscopy. Barium was then administered and flowed freely to the cecum. The barium was then drained and air insufflated into the colon. Multiple spot films of the colon were then obtained as well as overhead films of the abdomen.
FINDINGS: The scout film of the abdomen demonstrates a normal bowel gas pattern. No abnormal calcifications or evidence of bowel obstruction.
The barium flowed freely to the cecum with reflux into the terminal ileum. The caliber, haustral pattern and mucosal pattern of the colon is within normal limits. No pulps or masses. No strictures, filling defects or ulcerations. Spot views of the cecum demonstrate a normal ileocecal valve.
ERCP:
-
TECHNIQUE: Using a side-viewing endoscope, Dr. of the Gastroenterology Service cannulated the major papilla and injected water-soluble contrast. Multiple spot films were then obtained.
FINDINGS: Spot films are presented for interpretation. There is good filling of the intra and extra hepatic bile ducts. The bile ducts are of normal caliber. No areas of narrowing or filling defects are identified. (filling of the cystic duct and gallbladder. The gallbladder is grossly normal.)
The pancreatic duct was well filled from the head to the tail. This is of normal caliber. No filling defects, mass effect or narrowing.
INTRAVENOUS UROGRAM:
-
TECHNIQUE: A scout film of the abdomen was obtained. 75cc of omnipaque semi hundred was then administered intravenously. A 30-second nephrogram was obtained followed by serial overhead films of the abdomen at 5 and then 15 minutes were obtained. A post-void film was then obtained.
FINDINGS: The scout film of the abdomen demonstrates a normal bowel gas pattern. No abnormal calcifications or evidence of bowel obstruction.
The 30-second nephrogram demonstrates bilaterally symmetric nephrograms. The kidneys are normal in size, orientation, and enhancement. Serial delayed images demonstrate a non-dilated pelvicaliceal system and ureters bilaterally. No obstruction, calculi or filling defects are identified. The course of the ureters is normal. The bladder is well distended and the bladder wall is within normal limits. The post-void image demonstrates no significant post void residual.
CLINICAL HISTORY: 72-year-old male post-op prostatectomy for prostate cancer.
TECHNIQUE: Scout film of the pelvis was obtained. Approximately 150 ml of water soluble contrast was injected into the bladder via an indwelling catheter. Images in various projections were obtained. The bladder was then drained and a post-drainage image was obtained.
FINDINGS: Small contained leak at the base of the bladder on the right side. Miniscule amount of post-drainage residual urine. Minimal bladder trabeculae.
TECHNIQUE: A straight catheter was inserted into the distal urethra and water-soluble contrast was injected into it. Multiple spot films were then obtained in an oblique projection.
HYSTEROSALPINGOGRAM:
TECHNIQUE: The cervical os was cannulated by Dr. of the OB/Gyn Service. Water/soluble contrast was then administered and spot films of the pelvis were obtained.
FINDINGS: No mass lesions are identified in the endometrial canal. The walls of the uterus are smooth. Contrast material flows freely through the fallopian tubes and free spill into the peritoneal cavity is noted bilaterally.
IMPRESSION: Normal patent fallopian tubes bilaterally.
Ultrasonography
RIGHT UPPER QUADRANT ULTRASOUND:
-
TECHNIQUE:
Multiple axial and sagittal images of the right upper quadrant were obtained.
FINDINGS:
The visualized portions of the pancreas are within normal limits.
The visualized portions of the liver are also within normal limits. No focal lesions or intrahepatic bowel duct dilatation. The common bile duct is within normal limits in size measuring mms. The gallbladder is within normal limits. There is no gallbladder wall thickening, pericholecystic fluid or gallstones.
The visualized portions of the right kidney are within normal limits. No hydronephrosis.
KIDNEYS:
TECHNIQUE: Multiple sonographic images of the kidneys were obtained bilaterally and the axial and longitudinal planes.
FINDINGS: The kidneys are normal in size measuring approximately cms on the right and cms on the left in greatest longitudinal dimension. There is no hydronephrosis, abnormal calcifications, focal masses or perinephric fluid collections involving either kidney. The visualized portions of the bladder demonstrate no abnormalities.
SCROTAL ULTRASOUND:
-
TECHNIQUE: Multiple sonographic images of the testes were obtained bilaterally in the axial and longitudinal planes.
FINDINGS: The right testicle was normal in size measuring approximately x x cms. The echogenicity of the right testicle was homogeneous. No focal lesions or abnormal calcifications are identified. Blood flow to the testicle is within normal limits. The epididymis is also within normal limits.
The left testicle is normal in size measuring approximately x x cms. The echogenicity of the testicle is homogeneous. No focal lesions or abnormal calcifications are identified within the testicle. Blood flow to the testicle is normal. The epididymis is also within normal limits.
NEONATAL HEAD ULTRASOUND:
-
TECHNIQUE: Multiple sagittal and coronal images of the neonatal brain were obtained through the anterior fontanel.
FINDINGS: The ventricular system is normal in size bilaterally. There is no evidence of intracranial hemorrhage, mass effect or midline shift. No hydrocephalus. No anomalies are identified.
Procedure Notes
FLUOROSCOPICALLY GUIDED LUMBAR PUNCTURE (11/16/06):
CLINICAL HISTORY: 33-year-old female with history of pseudotumor cerebri. Status post lumboperitoneal shunt. Recently has been having recurrent headaches.
PHYSICIANS: Dr. K. Evans, Dr. E. Bourekas.
TECHNIQUE: The procedure and its associated risks were explained to the patient and informed consent was obtained.
The patient was positioned on the fluoroscopy table in the prone position. Using fluoroscopy, a suitable path for the lumbar puncture needle was determined. The skin was marked with a felt pen. The skin was then prepped and draped in the usual sterile fashion. The skin and underlying tissues were infiltrated with a total of 8 ml of lidocaine 1% without epinephrine.
Under fluoroscopic guidance, a 20-gauge lumbar puncture needle was inserted through the skin and into the lumbar cistern at the L3 level. Correct placement of the needle was confirmed by return of clear cerebrospinal fluid.
Opening pressure was determined, then 4 ml of cerebrospinal fluid was collected for analysis, then closing pressure was determined.
The stylet was re-inserted into the lumbar puncture needle and the needle withdrawn. Pressure was applied to the lumbar puncture site for 30 seconds. A Band-Aid was then applied to the site.
The patient was able to ambulate immediately. She tolerated the procedure well and there were no complications.
FINDINGS:
Opening pressure: 13 cm of water.
Closing pressure: 7 cm of water.
Amount of CSF removed: 4 ml - taken to the lab for cell count, and glucose and protein determination.
COMPLICATIONS: None.
IMPRESSION: Fluoroscopically guided lumbar puncture without complications.
I personally supervised the performance of this procedure and reviewed and approved the report.
-
CLINICAL HISTORY:
LUMBAR MYELOGRAM
-
TECHNIQUE: Informed consent was obtained. The lower back was prepped and draped in a sterile fashion. The skin was anesthetized with 1% lidocaine without epinephrine. Fluoroscopically guided lumbar puncture was performed at the L2-3 interspace level using a 20-gauge spinal needle. Approximately 12 cc of Omnipaque-180 was introduced into the thecal sac. The needle was removed. Multiple images of the lumbar spine were obtained in various projections.
FINDINGS: Minor impression on the thecal sac is noted at L5-S1, which may be related to a small disk osteophyte complex or a small protrusion. This will be further evaluated on the post-myelogram CT. The patient�s known sacral cyst does not demonstrate any opacification with contrast. The remainder of the exam is normal. There is no spinal stenosis. No obvious disk herniation is identified.
POST-MYELOGRAM CT OF THE LUMBAR SPINE
TECHNIQUE: Immediately following the myelogram, serial axial sections were obtained through the lumbosacral spine followed by sagittal and coronal reconstructions.
FINDINGS: At L5-S1, there is evidence of some osteophytic spurring off the posterior superior aspect of the S1 segment primarily centrally and on the left. There appears to be an associated small disk extrusion centrally, which causes minimal flattening of the thecal sac, however no spinal stenosis noted.
At L4-5, there is a minimal bulge of the annulus with no spinal or foraminal stenosis. The remainder of the examination is normal other than some minor degenerative changes of the L5-S1 facets.
ULTRASOUND-GUIDED LIVER BIOPSY:
-
CLINICAL HISTORY:
PHYSICIANS:
TECHNIQUE:
FINDINGS:
Three 18 gauge core biopsy specimens taken to lab in formalin
COMPLICATIONS: None.
IMPRESSION: Ultrasound-guided liver biopsy without complications.
I personally supervised the performance of this procedure and reviewed and approved the report.
TECHNIQUE: The procedure and associated risks were explained to the patient and informed consent was obtained.
The patient as positioned on the CT table in supine position and images were obtained in the subhepatic region. A suitable path for the drainage catheter was determined. The skin was marked with a felt pen. The skin was prepped and draped in the usual sterile fashion. The skin and underlying tissues were infiltrated with total of 5 cc of 1% lidocaine without Epinephrine.
The skin fascia was pierced with an 11 blade scalpel. A trocar needle was inserted down to the abscess. There was return of serosanguinous fluid. Correct positioning of the needle was confirmed by rescanning the patient. The needle trocar was removed and a guidewire inserted through the needle into the abscess. The needle was then withdrawn with the guidewire remaining in the abscess. Then dilators were inserted over the guidewire to dilate the tract for the drainage catheter. A 10 French pigtail catheter was inserted over the guidewire into the abscess. Correct positioning of the catheter was confirmed by return of fluid and by rescanning the patient. The end of the catheter was made into the curled up configuration so that it could not be pulled out. The other end of the catheter was secured to the patient's skin with an adhesive device. The catheter was then connected to a drainage bag. A specimen of the abscess fluid was sent to the lab for culture and sensitivity. A total of approximately 50 cc of fluid was drained during the procedure.
The entire site was then covered by a sterile op-site dressing and the patient was transported back to the ward in stable condition. Patient tolerated the procedure well. No complications.
IMPRESSION: CT-guided placement of drainage catheter in subhepatic abscess without complications.
I personally supervised the performance of this procedure and reviewed and approved the report.
Sample Chest Dictations
Sequence
Lungs (airways, pleura)
Lymph nodes
CVS
Abd
Bones
Chest wall
NORMAL
-
FINDINGS:
The lungs are clear bilaterally. No pulmonary nodules, consolidations, or pleural effusions.
No axillary, hilar, mediastinal, or paratracheal lymphadenopathy.
Heart size is normal. No pericardial effusion. Great vessels are unremarkable. No evidence of calcific coronary atherosclerosis or valvular calcifications.
Within the visualized upper abdomen, the liver, gallbladder, pancreas, spleen, kidneys and adrenal glands are within normal limits. No retroperitoneal or mesenteric lymphadenopathy. No free fluid or free air seen.
The visualized osseous structures are unremarkable. No suspicious sclerotic or lytic lesions observed.
Chest wall is unremarkable.
TECHNIQUE: After timed intravenous administration of a contrast bolus, contiguous axial slices with 2 mm and 5 mm collimation were obtained from lung apices to mid-kidneys. Right and left coronal oblique reconstructions done.
FINDINGS: The pulmonary arteries are well-opacified to the subsegmental level. No filling defects or other evidence of pulmonary embolism from the main pulmonary trunk to the subsegmental pulmonary arteries. Pulmonary trunk is of normal caliber.
CT AORTIC ANEURYSM STUDY
TECHNIQUE: Contiguous axial images from base of neck to ischial tuberosities both with and without contrast using 3 mm collimation and 1.5 mm collimation. Coronal and sagittal reconstructions as well as a 3D reconstruction of aorta and its branches.
FINDINGS: The prosthetic aortic graft extending from the base of the aorta to the hemi-arch is intact. No leakage observed.
Redemonstration of aortic dissection from distal end of the graft extending to the external iliac arteries bilaterally, at approximately the level of S1. The internal iliacs are not affected. Previously, the dissection extended to the T12 level. Therefore, this represents an extension of the dissection distally.
The dissection also extends superiorly to the left subclavian and left common carotid arteries. The right brachiocephalic trunk is not affected.
The true lumen is smaller than the false lumen and supplies most of the branches originating from the aorta. No identified compromise in perfusion to organs. The false lumen is also well opacified with contrast indicating significant blood flow.
TECHNIQUE:
-
Contiguous axial images using 5 mm collimation from lung apices to mid-kidneys following intravenous administration of contrast. B440 and B660 algorithms used.
Contiguous axial images using 5 mm collimation from lung apices to mid-kidneys following intravenous administration of contrast. Also, high-resolution CT of chest using 1 mm collimation at 10 mm intervals following intravenous administration of contrast.
FINDINGS:
-
Quality
-
Some images obtained during expiration and there is some motion artifact.
-
Endotracheal tube, right internal jugular central venous catheter in superior vena cava, nasogastric tube entering stomach, EKG electrodes stable and in satisfactory position.
Implantable cardioverter defibrillator is present in the right anterior chest wall with leads terminating in the right atrium and right ventricle.
ASD
-
There is redemonstration of lingular atelectasis and consolidation. There is also septal thickening in the right lung which may relate to edema or lymphangitic carcinomatosis.
-
Scattered areas of tree-in-bud centrilobular nodules and GGOs may relate to small airway disease.
Interval development of multifocal centrilobular nodules that are consistent with bronchiolitis.
Multifocal centrilobular nodules consistent with bronchiolitis affecting the right upper and middle lobes, and the lingula to a lesser extent. Associated bronchial wall thickening is also seen. Soft tissue infiltration surrounding the central right lower and middle lobe bronchi may relate to an infectious/inflammatory process, although malignancy cannot be excluded. Follow up CT recommended after appropriate antimicrobial therapy.
-
A 5 mm nodule is present in the right upper lobe (image 15) that is likely related to the adjacent pulmonary infection.
An irregular soft tissue nodule measuring 1.2 cm x 0.7 cm is located in the right upper lobe (image 23). It has a pleural tag. Although the spiculated features are worrisome, the lesion is likely benign given the patient's young age.
Pulmonary nodules identified on previous chest CT (12/04/2006) are stable. No new nodules seen.
Stable nodules, less than 3 mm in diameter, are present in the right upper lobe. These nodules have remained stable since the CT pulmonary angiogram in 6/05.
A calcified granuloma measuring 0.5 cm located in the lingula lobe is present. This is a benign lesion and requires no follow up.
Numerous scattered, small centrilobular nodules consistent with bronchiolitis, and a single small area of right basilar air-space disease are present and may have an inflammatory/infectious etiology.
-
Redemonstration of right lower lobe mass measuring 7.4 cm x 6.0 cm. A small amount of intra-tumoral gas is present, which may be indicative of cavitation or abscess formation. There may be direct extension of the mass into the mediastinum and/or adjacent lymph nodes since a tissue plane is not identified. The segmental bronchi are all patent. However the bronchus intermedius demonstrates an endoluminal, irregular soft tissue mass in the posterior aspect.
Possible etiologies include opportunistic fungal infection (such as zygomycosis) given patient's history of diabetes; and malignant neoplasm, such as bronchogenic carcinoma.
Redemonstration of infiltrative soft tissue mass involving the mediastinum and adjacent right hilum, and extending into the paratracheal, subcarinal, and precarinal spaces. It also appears to encase the main bronchi bilaterally. No endoluminal lesion seen. The lesion measures 6.5 cm x 4.8 cm (previously 7.4 cm x 5.0 cm).
Redemonstration of increasing mass effect on superior vena cava with stenosis and resultant prominent bronchial arteries and enhancement of the azygous system. There is focal mass effect by lymphadenopathy on the azygous vein (the pathologic lymph node measures 1.3 cm in short axis). There is mild improvement of the lumen of the right upper lobe bronchus from prior exam and even more marked improvement from the scan before that.
Redemonstration of postoperative changes consistent with left upper lobe wedge resection. Redemonstration of soft tissue mass at suture line in left upper lobe stable dating back to at least March 2006. This likely represents fibrosis or organized atelectasis. This could be further evaluated with PET/CT if concerned about local tumor recurrence.
Note is made of central soft tissue infiltration in the right tracheobronchial tree surrounding the central right lower lobe and middle lobe bronchi. This finding is new since the previous CT pulmonary angiogram done in 05/2006.
-
Nodular thickening of interlobar septa
Peribronchovascular thickening
Fissural nodualrity & thickening
Pleural effusions
Hilar lymphadenopathy
-
Bilateral scattered ground glass opacities likely related to inflammatory process. Cannot exclude hemorrhage.
Ground glass opacity in the right lower lobe may be post inflammatory. The walls of the right bronchial tree are mildly thickened.
-
Mosaic attenuation is demonstrated bilaterally with possible air trapping. This could relate to pulmonary artery hypertension or to distal airways disease given history of dyspnea.
Ill-defined centrilobular nodules, including tree in bud opacities, and acinar opacities in the right upper lobe, predominantly the posterior segment. To a lesser extent, these lesions are also found in the left lower lobe and right lower lobe.
Minimal basilar honeycombing consistent with subpleural basilar fibrosis or early usual interstitial pneumonitis.
-
Interlobular septal thickening
Intralobular reticular opacities
Traction bronchiectasis
Honey-combing
GGOs (prob dt fibrosis or alveolitis)
Architectural distortion
Mild mediastinal LAD
Predom juxtapleural zonees of lower lungs
Bronchi
-
Bronchiectasis and bronchiolitis are present in the left lower lobe.
Bilateral lower lobe bronchiectasis and bronchial wall thickening, with left side worse than right. Surrounding bronchiolitis present.
-
Tiny bilateral pleural effusions are present, with the left side larger than the right. This is likely secondary to recent intra-abdominal surgery.
-
Redemonstration of focal ovoid pleural lesion just posterior to the right lower lobe. It has attenuation of -1 Hounsfield units and measures 2.8 x 1.6 cm, which is stable from prior CT.
-
Bilateral multiple discontinuous foci of nodular pleural thickening, some of which exhibit intrinsic calcification. Bilateral calcified pleural plaques over the central tendinous portion of the hemidiaphragms consistent with asbestos-related pleural disease.
Lymph Nodes
-
No axillary, hilar, mediastinal, or paratracheal lymph nodes meeting size criteria for lymphadenopathy.
-
Heart size is normal. No pericardial effusion. Great vessels are unremarkable. Calcified atherosclerosis is present in the left anterior descending and circumflex arteries. Focal calcifications are observed in the aortic valve annulus.
The left anterior descending artery is mildly diffusely calcific consistent with atherosclerosis.
Calcific atherosclerosis is present in the left anterior descending artery.
There is also annular calcification of the mitral valve.
The pulmonary artery trunk measures 3.4 cm in diameter, suggestive of pulmonary artery hypertension.
-
The liver, gallbladder, pancreas, spleen and adrenal glands are within normal limits. There is no retroperitoneal or mesenteric lymphadenopathy. The visualized loops of small bowel and large bowel are within normal limits. No free fluid or free air within the visualized abdomen.
Indeterminate subcentimeter low-density lesion in the liver. Likely hemangioma or cyst.
Small low-density lesion in liver consistent with focal fatty infiltration, perfusion delay or cyst.
Within the abdomen, the gallbladder is absent and cholecystectomy clips are present.
There is likely splenomegaly with the spleen measuring 15.6 cm in the anterior-posterior direction, and 7 cm in the oblique dimension. There are no increased collateral vessels.
There is a renal cortical defect in the mid-pole of the left kidney, that likely relates to previous infection or infarction.
-
There is generalized osteopenia and generalized degenerative joint disease.
No suspicious sclerotic or lytic lesions.
Stable low-attenuation lesions with well-corticated borders are seen in a number of vertebral bodies.
Focal areas of osteopenia in the spine are stable.
The visualized spine exhibits degenerative changes at multiple levels. Noted are large anterior osteophytes.
-
A nodule measuring 3.3 x 2.4 cm is present within the left breast and is stable since the previous CT pulmonary angiogram.
An asymmetric soft tissue lesion is present in the right breast, measuring 3.5 cm x 1.8 cm, and exhibits spiculated borders. There is a small focus of calcification within it. This lesion is suspicious for breast cancer and correlation with mammography is recommended.
Post-surgical changes in the right axilla.
Redemonstration of asymmetric thyroid, with the right lobe larger than the left. The left lobe has a stable low density lesion.
IMPRESSION:
-
Air-space disease in lateral segment right middle lobe. If there are clinical findings consistent with pneumonia, an appropriate course of antimicrobial therapy followed by repeat chest radiograph six weeks post treatment is recommended. If the patient is currently asymptomatic, chest CT can be performed to exclude an endobronchial lesion.
Single pulmonary nodule. Repeat follow up CT scan in six months recommended to establish growth pattern and determine malignant potential.
A 4 mm pulmonary nodule is located in the right upper lobe adjacent to the chest wall. Given the patient's relatively high risk for lung cancer, and based on the nodule's size and current imaging recommendations, the nodule should be followed in twelve months to establish its growth pattern and determine malignant potential.
Mediastinal lipomatosis. No evidence of thymoma or thymic hyperplasia. Note that follicular thymic hyperplasia seen in patients with myasthenia gravis does not necessarily result in an imaging abnormality since it is a microscopic diagnosis.
Redemonstration of right middle lobe atelectasis. There is some mass effect on the middle lobe bronchus with distal obliteration. Bilateral multifocal patchy air space disease has shown interval worsening. Redemonstration of surrounding ground glass opacity. There is diffuse peribronchovascular thickening particularly along the central tracheobronchial tree. Redemonstration of scattered ground glass opacities predominantly in the lower lungs. bilateral septal thickening consistent with interstitial edema.
IMPRESSION:
Multi-focal nodular opacities are present predominantly in the lower lungs. Diagnostic possibilities include an inflammatory process or localized edema.
Stable right middle lobe atelectasis. There is mass effect on the middle lobe bronchus with distal obliteration of the bronchus. Endoluminal lesion cannot be exlcuded. Endoscopy can be performed for furher evaluation
Interval worsening of lingular air space disease. Some multi-focal nodular opacities predominantly in lower lungs and multi-focal ground glass opacities consistent with inflammatory process.
Interlobular septal thickening and new small right pleural effusion. Also peribronchovascular thickening along central tracheobronchial tree could relate to interstitial pulmonary edema. Recommend follow up.
*********************
The aorta extending from the root to the descending aorta is ectatic. The root measures 3.5 cm in diameter, ascending aorta 3.9 cm, descending aorta 2.9 cm. There is a small fusiform aneurysm off the distal abdominal aorta just proximal to the bifurcation and ectasia of the proximal common iliac arteries bilaterally. Extensive atherosclerosis is present. No evidence of dissection or ulceration of the posterior wall.
A large mass is present in the thorax encasing the descending aorta and effacing the esophagus. Left lower lobe bronchus is surrounded and left lower lobe is totally ectatic and consolidated. The left lower lobe pulmonary artery is totally encased.
Mild centrilobular emphysema with upper lobe predominance is present bilaterally.
The pulmonary artery is dilated measuring 3.8 cm in diameter suggestive of pulmonary artery hypertension.
The gallbladder is not seen and may be either contracted or removed surgically. Liver, pancreas, spleen, kidneys and adrenal glands are within normal limits. No retroperitoneal or mesenteric lymphadenopathy. The visualized loops of small and large bowel are unremarkable. No free air or free fluid within the abdomen or pelvis.
Degenerative disc disease is present at multiple levels in the spine with prominent anterior osteophytes.
IMPRESSION:
1. Small fusiform aneurysm of distal abdominal aorta. Ectasia of the thoracic aorta from root to descending aorta and ectasia of proximal common iliac arteries bilaterally.
2. Extensive atherosclerosis. Redemonstration of large mass and infarcts encasing the descending thoracic aorta, left lower lobe bronchus and left lower lobe pulmonary artery. Left lower lobe is atelectatic and consolidated.
3. Degenerative disc disease at multiple levels.
FINDINGS: Within the bronchus intermedius (image 58), there is a 2-3 mm density probably representing secretions. A less likely possibility is an endobronchial nodule.
IMPRESSION: Likely secretions in bronchus intermedius. Less likely possibility of endobronchial nodule. Recommend follow-up CT.
Within the lungs, there is mild interstitial edema (ground-glass opacity, peribronchial thickening, and septal thickening).
Sample Nuclear Medicine Dictations
-
F-18-FDG (FLUORODEOXYGLUCOSE) PET/CT (BODY), 1/29/07:
TECHNIQUE: Utilizing the Siemens Biograph-16 PET/CT imaging unit, PET, immediately preceded by transmission CT for attenuation correction and anatomic correlation, was obtained from the base of the skull to the mid thighs approximately 65 minutes after intravenous injection of 16.2 mCi of F-18-FDG.
FINDINGS: Previously demonstrated prevascular lesion is redemonstrated measuring 1.4 SUV max (previously 1.6 SUV). It is essentially stable.
In the aortopulmonary window there is a very tiny lymph node with no demonstrable hypermetabolism.
In the posterior medial portion of the liver there is artifactual small area of hypermetabolism. There is also nonspecific bowel activity. Hypermetabolism is also demonstrated in the nasopharynx and palatine tonsils. Clinical correlation is recommended. Mild increased activity in the salivary glands, likely inflammatory in nature.
Redemonstration of scarring versus atelectasis in the right upper lobe and to a lesser extent in the right middle lobe. No hypermetabolic lesions of note.
IMPRESSION:
1. Redomonstration of stable mildly hypermetabolic prevascular lymph node.
2. Hypermetabolism demonstrated in nasopharynx and palatine tonsils, likely infectious/inflammatory in nature. Clinical correlation recommended.
BREAST LESION LYMPHOSCINTIGRAPHY
CLINICAL HISTORY: 56 y/o female with right breast cancer.
TECHNIQUE: Four intradermal injections, each containing 107 uCi Tc-99m filtered sulphur colloid, were made at the 3, 6, 9, and 12 o'clock positions 1-2 cm from the margins of the lesion located in the right breast. No images were obtained. This was done at 9:50 a.m., 11/27/06, by Dr. Farrar for later surgical lymph node exploration using a gamma probe.
IMPRESSION: Radiopharmaceutic injection for intraoperative gamma probe detection.
CARBON-14 UREA BREATH TEST
TECHNIQUE: The patient swallowed a capsule containing 0.799 uCi carbon-14 urea. Ten minutes later, the patient exhaled into a balloon and the balloon was analyzed for carbon-14 labelled carbon dioxide gas.
FINDINGS: Relative to background radiation, the quantity of carbon-14 in the exhaled sample was -3 dpm (less than 50 dpm is considered negative for H. pylori infection).
IMPRESSION: Negative H. pylori carbon-14 urea breath test.
CHOLESCINTIGRAPHY with EJECTION FRACTION
TECHNIQUE: Views of the abdomen were obtained intermittently over a 60-minute period, after intravenous injection of 6.0 mCi Tc-99m-DISIDA. The patient then received 1.14 mcg of cholecystokinin intravenously and a gallbladder ejection fraction was calculated.
FINDINGS: The liver demonstrates homogeneous intensity. There is visualization of extrahepatic bile ducts and gallbladder within 10 minutes and intestinal activity at 15 minutes.
Gallbladder ejection fraction calculated to be 18% (normal is greater than 40%).
IMPRESSION:
1. Decreased gallbladder ejection fraction, consistent with chronic cholecystitis.
2. No evidence of biliary obstruction.
CUTANEOUS LYMPHOSCINTIGRAPHY
TECHNIQUE: Four intradermal injections of 107 uCi Tc99m filtered sulphur colloid in 0.1ml of normal saline each were made at the 3, 6, 9, and 12 o'clock positions 1-2 cm from the margins of the surgical site located on the patient�s back. Images of the left axilla were obtained intermittently over a 60-minute period, and the sentinel nodes marked with indelible ink prior to sending the patient to surgery.
FINDINGS: The first lymph node was demonstrated by the radiotracer at 5 minutes and was located in the superior lateral aspect of the left axilla. The next two lymph nodes appeared at 10 minutes and were located approximately 3 cm and 6 cm inferior to the first lymph node, respectively.
IMPRESSION: Sentinel lymph node identification and marking for intraoperative detection.
DUAL WHOLE BODY BONE SCAN & INDIUM-111 WHITE BLOOD CELL SCINTIGRAPHY
TECHNIQUE: Multiple spot scintigraphs in various projections were obtained following IV injection of 10.9 mCi Tc-99m MDP and 0.50 mCi indium-111 labeled autologous white blood cells. Angiogram, blood pool, and three hour delayed images were obtained.
FINDINGS: The white blood cell scan demonstrates no foci of increased activity.
The bone scan demonstrates minimally increased general flow to the right foot relative to the left. On the blood pool phase and the delayed phase, the distal end of the left first metatarsal demonstrates increased activity. The right foot demonstrates no foci of increased activity on the blood pool or the delayed images.
IMPRESSION:
1. No evidence of osteomyelitis.
2. Right foot demonstrates subtle increase in flow relative to left foot. Clinical correlation recommended.
3. Increased activity at the distal end of the left first metatarsal, which may represent postoperative or degenerative change.
GASTRIC EMPTYING NUCLEAR MEDICINE STUDY, 11/20/06:
COMPARISON EXAMINATION: None.
CLINICAL HISTORY: 61-year-old female with diabetes mellitus. Complains of fullness and loss of appetite.
TECHNIQUE: Following ingestion of 1.00 mCi of Tc-99m Chelex resin in one ounce of unsweetened instant oatmeal and reconstituted to a total volume of six fluid ounces with water, serial images with the images in supine position utilizing the posterior projection were obtained over a 45-minute period. The half-life of gastric emptying was calculated.
FINDINGS: The calculated half-life of gastric emptying was 31 minutes (normal range 24-48 minutes).
Some radiotracer is observed in the distal esophagus. This likely represents esophageal dysmotility, although gastroesophageal reflux is a possibility. A barium swallow is recommended to further evaluate this.
IMPRESSION:
1. Normal gastric emptying.
2. Esophageal dysmotility or gastroesophageal reflux.
e.g. Focal esophageal retention of radiotracer is seen for the majority of the study. Esophageal functional or structural pathology such as dysmotility or diverticulum are possible explanations.
I personally viewed and interpreted these images and I have reviewed and approved this report
IODINE-131 ADMINISTRATION FOR THYROID CANCER, 11/29/06
COMPARISON EXAM: Iodine-131 whole-body scintigraphy 11/29/06.
CLINICAL HISTORY: 22-year-old female status-post thyroidectomy for thyroid cancer.
TECHNIQUE: The patient received 50.4 mCi sodium iodide solution orally as therapy for thyroid cancer. The radiopharmaceutical was administered under the supervision of Laura Ryan, M.D. No images were obtained.
IMPRESSION: Radioiodine-131 administration for thyroid cancer.
RADIONUCLIDE GFR
TECHNIQUE: Utilizing 8.8 mCi Tc-99m DTPA IV, the callibrated gamma camera, Gate's technique, and computer-derived renal depths; split renal function and GFR were determined.
FINDINGS: Total GFR was 28 ml/min. Normalized GFR was 27 ml/min.
Split renal function revealed that the right kidney provided 48% and the left kidney provided 52% of total GFR.
GI HEMORRHAGE LOCALIZATION STUDY
TECHNIQUE: Cine and intermittent images of the abdomen and pelvis were obtained over a 2 hour period following the intravenous injection of 25.0 mCi of technetium-99m in vitro labeled autologous red blood cells.
FINDINGS: No evidence of abnormal activity collection within the abdomen and pelvis to suggest active GI bleeding. Splenomegaly is present. Collateral vessels are present in the abdomen and pelvis.
IMPRESSION: No evidence of GI bleeding during the time course of the study.
INDIUM-111 WHITE BLOOD CELL SCINTIGRAPHY
TECHNIQUE: Whole body scintigraphs were obtained 24 hours after IV injection of 509 microcuries of indium-111 labeled autologous white cells.
FINDINGS: There is an area of focal white blood cell accumulation in the left mid chest seen more prominent on the posterior view and probably within the lung. This is suspicious for a focus of infection in the left lung.
The spleen is diffusely enlarged. The liver is prominent.
There is bone marrow expansion in the distal femurs, proximal tibia, pelvis, and proximal humeri. Of note is asymmetry in the proximal humeri, with the right humerus being more intense than the left, uncertain significance and clinical correlation is recommended.
IMPRESSION:
1. Focal white blood cell accumulation in the left mid chest region seen more prominent on posterior view , suspicious for lung infection when correlating with chest CT findings.
2. Splenomegaly.
3. Diffuse bone marrow expansion. Slightly assymetric bone marrow distribution in proximal humeri, is of uncertain significance. Clinical correlation recommended.
IODINE-131 WHOLE BODY SCINTIGRAPHY
TECHNIQUE: 48 hours after ingestion of 2.06 mCi of I-131 sodium iodide, whole body scintigraphs, spot views of the neck and chest, pinhole view of the neck plus radioactive iodine neck uptake determinations were performed.
FINDINGS: Uptake is present in the thyroid bed bilaterally; however, the images are compromised by patient motion. Uptake in the remaining parts of the body are physiologic.
At 48 hours, there is 0.23% retention in the neck and 9.5% total body retention.
IMPRESSION: Bilateral thyroid bed uptake. No evidence of metastatic disease in lateral neck compartments or distant sites.
QUANTITATIVE PULMONARY PERFUSION STUDY
TECHNIQUE: Utilizing 5.0 mCi Tc-99m MAA intravenously, dividing the lungs into thirds in a craniocaudad direction, utilizing simultaneous anterior and posterior projections (750,000 counts per posterior projection), and a geometric mean method; relative perfusion to various regions of the lungs were calculated.
FINDINGS:
Right upper lung: 15%
Right middle lung: 33%
Right lower lung: 14%
Total right lung lung: 61%
Left upper lung: 11%
Left middle lung: 20%
Left lower lung: 8%
Total left lung lung: 39%
RENAL TRANSPLANT SCAN
TECHNIQUE: Dynamic perfusion and functional images of the transplanted kidney were obtained for 20 minutes following IV bolus injection of 10.9 mCi Tc 99m MAG3.
FINDINGS: There is normal perfsuion of the transplanted kidney in the right pelvis. Persistent cortical retention of tracer is noted without any observed excretion into the bladder. Collecting system is obscured by intense parenchymal activity. However, some activity is noted in the urinary collection bag indicating some excretion.
A photopenic area is observed superior to the transplanted kidney. This may represent a hematoma, urinoma, lymphocele, seroma, or other postoperative fluid collection. See ultrasound study done 11/20/06.
IMPRESSION:
1. Normal perfusion with significant parenchymal retention of activity and mild excretory function , suggestive of acute tubular necrosis of transplanted kidney.
2. Photopenic area superior to transplanted kidney likely consistent with postoperative fluid collection.
THYROID UPTAKE & SCAN
TECHNIQUE: Radioactive iodine thyroid uptake (RAIU) determinations were performed at approximately 6 hours and 24 hours post ingestion of 242 mC of I-123 in capsule form. Thyroid scintigraphs were then obtained.
FINDINGS: The thyroid scintigraphs demonstrate diffuse enlargement of the thyroid gland and diffusely increased activity. There is a photopenic area at the medial base of the right lobe. This is likely a colloid cyst or thyroid nodule (see previous ultrasound scan report).
Mean uptake at 6 hours was 46.9% (normal range is 5-12%). Mean uptake at 24 hours was 58.3% (normal range is 7-33%).
TRIPLE PHASE BONE SCINTIGRAPHY of DISTAL UPPER EXTREMITIES
TECHNIQUE: A radionuclide angiogram followed by blood pool images and three-hour delayed static views of the distal upper extremities in various projections were performed following intravenous administration of 25.4 mCi of technetium-99m MDP.
VENTILATION / PERFUSION SCAN
TECHNIQUE: A ventilation study was performed utilizing Tc-99m DTPA aerosol (42 mCi in nebulizer) followed by pulmonary perfusion study utilizing 5.22 mCi Tc-99m MAA intravenously. Chest radiograph was done within 30 minutes of the V/Q study and was available for correlation.
FINDINGS: Small matched defects are present in the right lung base anteriorly, right anterior upper lung, left anterolateral lung base. Soft-tissue attenuation likely accounts for much of these findings (the patient weighs approximately 300 pounds).
IMPRESSION: Low probability for pulmonary embolism.
WHOLE BODY BONE SCAN, 11/20/2006:
COMPARISON EXAM: CT abdomen with contrast, 11/20/2006; CT chest with contrast, 11/20/2006; whole body bone scan 4/3/2006.
CLINICAL HISTORY: 57-year-old female with history of metastatic breast cancer.
TECHNIQUE: Whole body scintigraphs were obtained approximately 3 hours post intravenous injection of 25.0 mCi of technetium 99m-MDP.
FINDINGS: Stable diffuse increased activity is observed within the skull. Increased activity is also present in L1 and L5, with L5 being more prominent than on the previous study. However, a contrast enhanced CT done the same day indicates that the lesions are stable.
Increased activity is noted involving the right mandible, which is likely secondary to dental pathology. There is also increased activity at the left sternoclavicular joint, angle of the sternum, and xiphoid process, which are likely due to degenerative disease. This is confirmed on the contrast enhanced chest CT done the same day. Stable degenerative changes are also noted in the shoulders and knees bilaterally and in the right first metatarsophalangeal joint.
Diffuse increased activity is observed in the skull, which is stable and is likely a normal variant
IMPRESSION:
1. Stable metastases involving L1 and L5.
2. Diffuse increased activity in skull, which is stable and is likely a normal variant.
3. Stable degenerative changes at multiple locations.
Nuclear Medicine Gamuts


Brain
Tc-99m pertechnetate-HMPAO, Tc-99m ECD, N-13-ammonia (PET) are perfusion agents, lipophilic & extracted on first pass.
Diamox → vasodilation of Nl areas → worsened perfusion in areas of vascular dz.
Tl-201, F-18-FDG (PET) are metabolic agents with activity in tumors but not in areas of radiation necrosis.
Indium-111-DTPA intrathecally for CSF leak or NPH.
| Multiple, asymmetric cortical perfusion defects | Multi-infarct dementia, vasculitis, coccaine abuse |
| Symmetrical ↓ activity in posterior parietal-temporal lobes; preserved activity in calcarine cortex & basal ganglia | Alzheimer's dz (not specific) |
| ↑ activity temporal lobe | Herpes encephalitis |
| ↑ perfusion & ↑ metabolism during seizure; ↓ or Nl activity interictally | Seizure focus |
| Lack of intrathecally-administered Indium-111-DTPA activity superior surface of brain after 1-2 days | Indicates NPH |
Thyroid
| Tc-99m pertechnetate | IV | trapped |
| Radio-iodine, e.g. I-123 | PO | trapped & organified |
Discordant nodule: Some Ca are hot using Tc-99m pertechnetate & cold using I-123.
Thyrotoxicosis
| Condition | %RAIU | Scan | |
| Grave's dz | ↑ | Enlarged, homogeneous | |
| Toxic multinodular goitre (Plummer's dz) | hi Nl or ↑ | Hyperfunctioning nodules, suppressed extra-nodular tissue | |
| Hashitoxicosis (rare, transient) (chronic thyroiditis) (lymphocytic infiltn) | ↑ | Enlarged, patchy | |
| Toxic nodule (adenoma) | usu. Nl | Hyperfunctioning nodule, suppressed extra-nodular tissue | |
| Subacute thyroiditis E.g. de Quervain's (granulomatous) thyroiditis, silent thyroiditis, post-partum thyroiditis | ↓ | Nonvisualization | |
| Struma ovarii (functioning thyroid tissue in ovarian teratoma) | |||
| ↓ | |||
| ↓ | |||
| ↓ |
GI
Hepatobiliary
Tc-99m IDA (e.g. DISIDA) is excreted by hepatocytes, but not conjugated.
indicates
| Non-visualization of GB at 4 hrs or after morphine at 1 hr | likely acute cholecystitis |
| rim sign | may be gangrene, rupture, abscess |
| Non-visualization of GB at 1 hr but visualization at 4 hrs or after morphine | likely chronic cholecystitis |
| Persistent cardiac blood pool activity, poor liver activity, & no biliary excretion | hepatocellular disease (e.g. hepatitis, cirrhosis); severe biliary obstruction |
| No bowel activity by 1 hr | Common duct calculus, tumor, stricture, morphine, sphincter dyskinesia, chronic cholecystitis |
| Only liver activity & no cardiac, biliary , or bowel activity | may be "liver scan of complete biliary obstruction" |
| In neonate, no bowel activity by 24 hrs | biliary atresia, severe hepatitis |
| CCK ejection fraction | > 50% normal 35 - 50% borderline <35% abnormal - sugg acute or chronic cholecystitis |
Colloid Liver-Spleen
Tc-99m sulfur colloid
| Colloid shift: BM easily visualized; spleen activity > liver | Hepatocellular disease ( also look for ascites, hepatoma (photopenic)) |
| Photopenic lesions | Anything that not have reticuloendothelial activity (e.g. liver: cyst, hematoma, abscess, fatty infiltration, adenoma, hepatoma, mets e.g. spleen: cyst, tumor, infarct) |
| ↑ activity | FNH, regenerating nodule in cirrhosis, flow abnls |
Meckel's Diverticulum Imaging
Tc-99m pertechnetate (concentrates in gastric mucosa, in stomach or ectopic)
Pentagastrin → ↑ mucosal uptake of Tc-99m pertechnetate
Cimetidine → block release of Tc-99m pertechnetate from mucosa
Glucagon → ↓ small bowel motility
GI Bleeding Study
Tc-99m-labelled RBC's (Tc-99m sulphur colloid only if active bleeding)
GU
Kidneys
Tc-99m-DTPA: GFR
Tc-99m-DMSA: renal cortex
Tc-99m-MAG3: tubular agent
Tc-99m-glucoheptonate: renal cortex & collecting system
| Tc-99m-MAG3 → delayed clearance with signif cortical retention | Renal artery stenosis |
| Tc-99m-MAG3 → bilateral delayed clearance with signif cortical retention | Bilateral renal artery stenosis, obstruction, medical renal dz, pre-renal azotemia |
| Tc-99m-MAG3 or DTPA → delayed clearance (20 - 30 mins) with dilated intrarenal collecting system | Flaccid system or obstruction. If furosemide → rapid washout, then probab flaccid system. |
| Tc-99m-MAG3 → Nl perfusion, ↑'g cortical activity, ↑'g renograms | ATN, cyclosporin toxicity |
| Tc-99m-MAG3 → absent perfusion | Hyperacute rejection (< 24 hrs post-transplantn) |
| Tc-99m-MAG3 → poor perfusion, poor excretion | Acute rejection (2 -3 mos post-transplantn) |
Testes
| Diffusely hot | Epididymitis |
| ↓ or absent testicular flow | Torsion |
Adrenal
| NP-59 → unilateral adrenal cortical uptake | Usu adenoma |
| NP-59 → bilateral adrenal cortical uptake | Usu hyperplasia |
| MIBG → tissue localization | pheochromocytoma, neuroblastoma, paraganglioma, carcinoid, medullary thyroid Ca |
Respiratory
Modified PIOPED Criteria
| Probability | Criteria | ||
| High (> 80%) | >= 2 large mismatched segmental perfusion defects or the arithmetic equivalent | ||
| Intermediate (20% - 80%) | One moderate to < two large mismatched perfusion defects or the arithmetic equivalent Single-matched ventilation-perfusion defect with a clear chest radiograph is borderline for low probability Difficult to categorize as low or high | ||
| Low (<20%) | Nonsegmental perfusion defects (e.g.cardiomegaly, enlarged aorta, enlarged hila, elevated diaphragm) Any perfusion defect with a substantially larger chest radiographic abnormality Perfusion defects matched by ventilation abnormality provided that there are: a) clear chest radiograph; and b) some areas of normal perfusion in the lungs Stripe sign Any number of small perfusion defects with a normal chest radiograph | ||
| Very Low | <= 3 small perfusion defects ("rat bites") | ||
| Normal | No perfusion defects or perfusion exactly outlines the shape of the lung seen on the chest radiograph |
Segmental perfusion defects:
Large = >75%
Moderate = 25% - 75%
Small = <25%
Chest Radiology Gamuts
| Normal | Else
|
|
| Highest level of dome of diaphragm > 1.5 cm above line b/n costophrenic & vertebrophrenic junctions
| Empysema
| Paratracheal stripe < 10 mm
| CHF, lymphoma, bronchogenic cyst
| Main PA < 3 cm
| Indicative of PA hypertension
| Aorta: | Root < 3.6 cm Ascending < 3.5 cm Proximal descending < 2.6 cm Distal descending < 2.4 cm Abd < 3 cm Aneurysm | |
PA
Major fissure visible → ipsilateral lower lobe atelectasis
H/o breast Ca → look for internal mammary LAD; vertebral metastases
H/o lymphoma → look for donut sign on lateral CXR
Cavity wall:
< 5 mm → infection
> 10 mm → SCC
Autoimmune Diseases
| I | asthma |
| I & II | allergic bronchopulmonary aspergillosis |
| II | Goodpasture's Sx |
| III & IV | hypersensitivity pneumonitis |
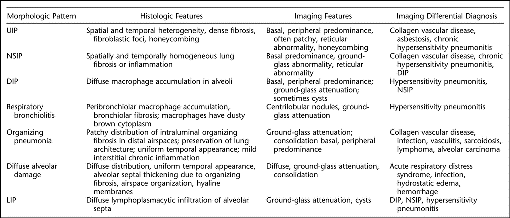
Links
CT-based delineation of lymph node levels in the Neck
University of Washington Department of Radiology
Grainger & Allison's Diagnostic Radiology
Cervical Spine Radiographs in the Trauma Patient
CPI Modules
ke05051017
TMC Emergency Radiology Primer
Musculoskeletal Radiology Differential Diagnosis